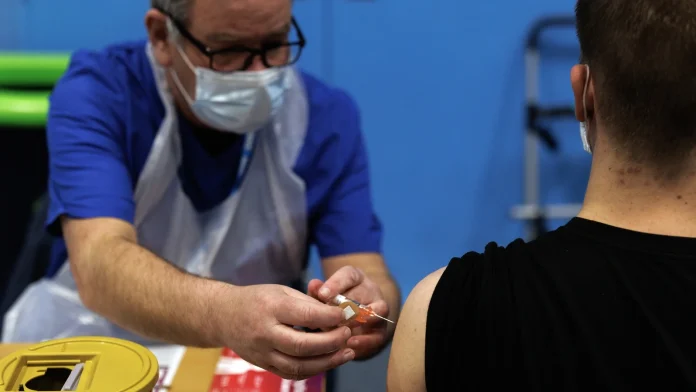
When a Night Out Becomes a Global Wake-Up Call
It began like any Saturday in a seaside town: loud music, neon flashes, bodies pressed shoulder to shoulder on a dance floor. Within days of that night, two people were dead, and more than 10,000 residents in Kent, England, turned up at clinics to be vaccinated against a disease that most of us imagine belongs to history books and crowded clinics in distant lands.
That abrupt, local panic is the kind of moment that makes the headlines. But a new, sweeping analysis — published in Lancet Neurology and compiled by the Institute for Health Metrics and Evaluation (IHME) — pulls the curtain back and shows us a quieter, lonelier toll playing out across continents.
More than a Quarter of a Million Lives Lost
The IHME team estimates that in 2023 some 259,000 people died from meningitis worldwide. Children accounted for roughly one in three of those deaths. Those numbers are not just statistics on a page; they represent hospitals clogged with fevered infants, rural clinics struggling with scarce antibiotics, and grieving families in cities, towns and villages from Europe to West Africa.
“When you see a child with the rash and the stiff neck, you know that every minute matters,” said Dr. Mariam Okoye, a pediatric infectious disease specialist who has worked in clinics across West Africa. “But in many places the nearest hospital is hours away, and often there aren’t the diagnostics or intensive care beds to make a difference.”
Where the Burden Concentrates
The IHME study points to the African meningitis belt — a swath of countries stretching from Senegal in the west to Ethiopia in the east — as the region with the highest rate of cases. Nigeria, Chad and Niger were singled out as particularly affected.
That geography is no accident. For decades this semi-arid band has seen cyclical waves of bacterial meningitis, especially during the dry Harmattan season when dust, cold nights and mass gatherings (markets, weddings, pilgrimages) create a perfect storm for transmission.
“In the villages, funerals and market days bring people together from miles around,” explained Souleymane, a market trader in central Niger. “We don’t want to stop our lives, but when an illness starts, it spreads fast.” His voice carried the weary pragmatism of someone who has watched outbreaks ripple through tight-knit communities.
How Meningitis Kills — and Why It Is So Hard to Track
Meningitis is an inflammation of the membranes covering the brain and spinal cord. It can be caused by viruses, bacteria, fungi or parasites. The distinction matters: viral meningitis is generally more common and less deadly, whereas bacterial meningitis is rarer but far more lethal and more likely to leave survivors with permanent disabilities.
Globally, bacterial meningitis has one of the highest case-fatality rates among common infectious diseases. Even with timely treatment, death rates can be 10–20 percent; without prompt care, they can climb much higher. Survivors may experience hearing loss, cognitive impairment or motor disabilities.
“Too many deaths are hidden in places where people never reach the health system,” said Dr. Ana Paredes, an epidemiologist involved with global surveillance networks. “Underreporting is a major obstacle. If cases and deaths aren’t recorded, they don’t trigger the resources needed to prevent the next outbreak.”
Risk Factors: From Birth to Breathing
The IHME analysis flagged several risk factors that increase vulnerability: low birthweight and premature birth, which compromise newborns’ immune systems, and perhaps more surprisingly to many readers, air pollution.
Airborne particles—whether from cooking fires inside homes, traffic in crowded cities, or dust storms in the Sahel—can inflame the respiratory tract and make it easier for bacteria to move from the nose and throat into the bloodstream and then into the protective membranes of the brain.
“We are starting to see infectious disease and environmental health conversations overlap,” noted Dr. Priya Menon, a public health researcher focusing on air quality and infectious diseases. “Wherever you scratch the surface of health, the social determinants—poverty, housing, pollution—are right there.”
Progress, but Not Fast Enough
There are reasons to be hopeful. Since 2000, expanded vaccination campaigns have dramatically reduced some forms of meningitis. The MenAfriVac campaign, for instance, nearly eliminated devastating group A meningococcal epidemics in many parts of the African belt.
Yet the IHME study warns that the World Health Organization (WHO) is unlikely to meet its 2030 targets unless efforts accelerate. The WHO aims to cut bacterial meningitis cases by 50 percent and deaths by 70 percent from 2015 baselines by the end of the decade. According to the analysis, current declines are occurring at only about half the speed required.
“We need scaled-up immunisation, better access to care, and stronger diagnostics and surveillance—especially in low-income countries,” the study stresses. “Without that, targets will be missed.”
Local Responses, Global Signals
In Kent, the sudden push to vaccinate more than 10,000 people after the nightclub-linked bacterial outbreak was a rapid, visible response. “We were terrified, but the clinics were organized and calm,” said Emma Clarke, 28, who received the vaccine. “I thought, why haven’t we talked about this more?”
Her question is the one public health officials worry about: awareness is often reactive. Vaccines are powerful tools, but they reach people unevenly—stymied by supply constraints, competing priorities, misinformation, and fragile health systems.
“The story of meningitis is also a story about health equity,” said Dr. Okoye. “When children die in our wards, it’s usually because of delays that would not happen in better-resourced settings.”
What Can Be Done — and What You Can Ask
The path forward is both technical and moral. It includes expanding vaccine coverage across all relevant bacterial strains, strengthening laboratory networks so cases are quickly detected and characterized, and investing in primary health care so families can reach care before it is too late.
Policy changes can be costly; political will can be fickle. But incremental actions—improving prenatal care to reduce low birthweight, combating indoor air pollution, funding community health workers—add up.
So ask yourself: how does your country prioritize infectious disease prevention? Are the vulnerable populations in your community—newborns, the elderly, people living in polluted neighborhoods—seen and counted? What would it take for leaders to treat meningitis not as an occasional headline but as a continuous priority?
From Headlines to Lasting Change
Outbreaks in an English nightclub or a market in Niamey are not merely isolated tragedies; they are interconnected signals of a global system still struggling to close gaps. The IHME report is blunt: progress is real, but insufficient.
“This is a preventable tragedy in many cases,” Dr. Paredes said. “We have the vaccines and the tools. What we lack in many places is reach and resilience.”
If anything, the recent surge of attention—sparked by deaths far from the traditional hotspots—should be a prompt: to invest in surveillance, to broaden vaccine access, and to remember the mothers and fathers who lose a child to a disease that could often have been stopped.
We can read the numbers and nod. Or we can listen to the markets, the clinics, and the exhausted nurses and choose differently. Which will we choose?